A kidney finding on a scan can feel unsettling, especially when the report mentions a "cyst", a "mass", or a "lesion". Those words can sound similar, yet they do not mean the same thing. In day-to-day practice, many kidney cysts are harmless and need little more than reassurance, while kidney tumours demand a very different level of attention.
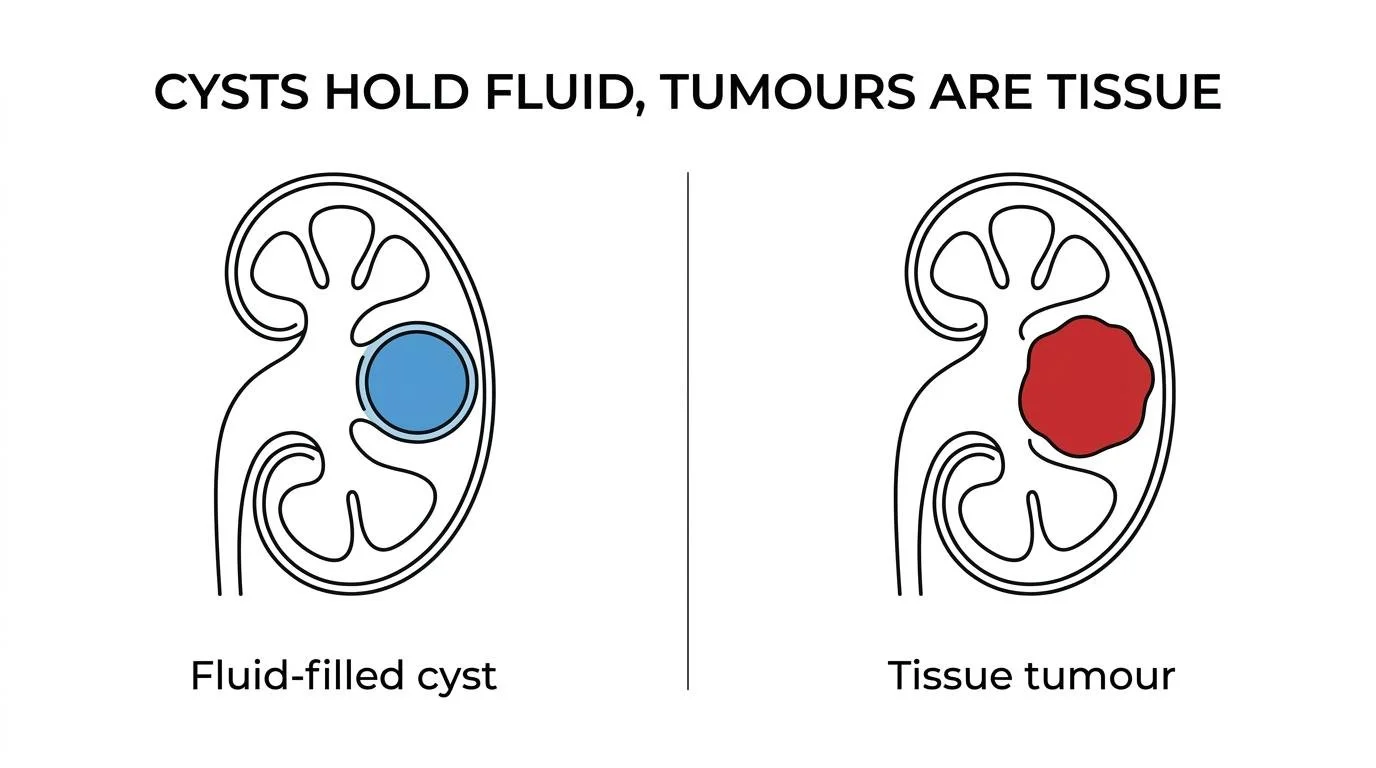
The key distinction is structural. A cyst is usually a fluid-filled sac. A tumour is an abnormal growth of tissue. The difficulty comes from the grey area between the two — some kidney tumours can appear partly cystic on imaging, and some cysts are more complex than a simple fluid pocket. That is why imaging quality and specialist interpretation matter so much.
Most kidney cysts found incidentally on scans are entirely benign and require no treatment. Kidney cysts become more common with age — many people discover them incidentally during scanning for an unrelated reason. The important question, which imaging can usually answer clearly, is whether what has been found is a simple cyst or something that needs closer attention.
The basic difference — cyst versus tumour
A simple kidney cyst is typically a round or oval pocket of fluid enclosed by a thin, smooth wall. These are very common, particularly in older adults, and the vast majority behave entirely benignly. They rarely cause symptoms, do not behave like cancer, and in most cases need no follow-up once confirmed as simple on good-quality imaging.
A kidney tumour is different. It consists of cells growing abnormally within the kidney. Some kidney tumours are benign — angiomyolipoma and oncocytoma are the most common benign solid tumours — but the ones that require urgent attention are malignant tumours, particularly renal cell carcinoma, which accounts for the vast majority of adult kidney cancers.
| Feature | Kidney cyst | Kidney tumour |
|---|---|---|
| Basic structure | Fluid-filled sac with a thin wall | Abnormal tissue growth — solid or mixed solid/cystic |
| Usual behaviour | Usually benign | Benign or malignant — requires characterisation |
| Appearance on imaging | Thin smooth wall, no solid component, no contrast enhancement | Solid or partly solid tissue, enhances after contrast |
| How common | Very common — increases markedly with age | Less common |
| Typical management | Often none required | Depends on type, size, and staging |
| Urgent specialist review | Usually not required if clearly simple | Yes — prompt urology assessment advised |
The language of radiology reports can make this confusing. A report may describe a "renal mass" — and that term encompasses both cysts and tumours. The critical next question is always: what type of mass is it?
Symptoms — and why most are found by chance
One of the most clinically important features of both kidney cysts and kidney tumours is that they are very often completely silent. Many are discovered incidentally during scans performed for an unrelated reason — back pain, kidney stones, abdominal discomfort, or a routine health check. This is particularly true of small and medium-sized lesions.
When symptoms do occur, they can overlap significantly between cysts and tumours:
- Blood in the urine — raises more concern for a tumour, but does not confirm cancer on its own; should always prompt investigation
- Flank or back pain — a large cyst or tumour can cause discomfort in the loin or upper abdomen
- Fever and tenderness — can indicate an infected cyst, which requires specific treatment
- Unexplained weight loss or tiredness — more associated with advanced tumours than benign cysts
- A palpable abdominal mass — uncommon but a reason for urgent review
Symptoms can suggest a direction, but they rarely settle the diagnosis by themselves. The real distinction almost always comes from imaging.
What imaging shows — and why the details matter
Ultrasound is usually the first imaging investigation. A simple cyst looks black on ultrasound — sound waves pass straight through fluid — and has a thin, smooth, featureless wall with no solid components. When a lesion does not fit this pattern, or when ultrasound cannot characterise it fully, the next step is CT or MRI with contrast.
CT and MRI provide far greater detail. Radiologists evaluate the wall thickness, any internal divisions (septa), calcification, solid components, and critically — whether the lesion enhances after intravenous contrast. Enhancement indicates blood supply and living tissue rather than simple fluid, and pushes a finding towards a tumour rather than a harmless cyst.
This distinction becomes especially important with complex lesions. Some kidney cancers are not fully solid — they can be partly cystic, with thick septa or a nodule on the wall. That is why a report may describe a lesion as "complex cystic" — a category that sits between a clearly benign cyst and a clearly solid tumour, and which has its own classification system.
Simple cyst: thin smooth wall, fluid density, no solid component, no measurable enhancement after contrast. Suspicious tumour: enhancing tissue, thick or irregular wall, septa that enhance, or mural nodules. Indeterminate: features that are not clearly benign — requires repeat imaging, MRI, contrast-enhanced ultrasound, or in selected cases biopsy.
The Bosniak classification — how complex cysts are graded
When a kidney lesion appears cystic rather than clearly solid, specialists use the Bosniak classification to communicate how concerning it looks on imaging and to guide management. The system was recently updated, but the principle remains the same: higher categories carry a greater chance of malignancy and prompt more active management.
A Bosniak I cyst and a Bosniak IV lesion can both be described as "cystic" on a scan report — yet the clinical implications are completely different. Understanding where on this scale your lesion sits is the most important single piece of information after a complex kidney finding.
Told you have a kidney lesion or mass?
Mr Sri accepts referrals for kidney lesions of all complexities — including second opinions for patients uncertain about their imaging findings or management plan.
Causes — why cysts and tumours arise differently
Simple kidney cysts are linked primarily with ageing rather than cancer biology. Their exact cause is not fully understood, but they become progressively more common in older adults — by the age of 70, many people have at least one. They appear to arise from degenerative changes in tubular structures within the kidney rather than from any cancer-related process.
Kidney tumours have a distinct risk profile. The established risk factors for renal cell carcinoma include smoking, obesity, hypertension, chronic kidney disease, and specific inherited syndromes including Von Hippel-Lindau disease. Men are approximately twice as likely as women to develop kidney cancer. Family history matters, particularly for inherited conditions, though most renal cell carcinoma is sporadic rather than hereditary.
Treatment — how cysts and tumours are managed differently
Most simple kidney cysts need no treatment whatsoever. If a cyst is not causing pain, infection, obstruction of the collecting system, or pressure on adjacent structures, it is left alone. This is one of the most genuinely reassuring outcomes in kidney medicine.
If a simple cyst does cause symptoms, options include aspiration (draining the cyst) or surgical deroofing using a minimally invasive approach. The goal is relief of symptoms, not cancer treatment.
Kidney tumours are managed along a different pathway entirely:
For advanced kidney cancer that has spread beyond the kidney, the treatment landscape has improved substantially over the past decade. Modern immunotherapy combinations and targeted agents have meaningfully extended survival for many patients with metastatic disease.
Prognosis — the importance of what type of lesion it is
The outlook for a confirmed simple kidney cyst is excellent — once clearly characterised as Bosniak I or II, it requires no follow-up in most cases and carries no cancer risk. Bosniak IIF lesions are typically watched with interval imaging and frequently remain stable indefinitely.
For kidney tumours, prognosis depends strongly on stage at detection. Localised tumours — particularly small ones found incidentally — are often curable with surgery. Partial nephrectomy for tumours under 4 cm carries a very low recurrence risk in experienced hands. The picture is more serious for advanced or metastatic disease, though treatment outcomes have improved considerably.
Modern imaging has made this entire pathway far clearer than it was even ten years ago. Most patients who receive an unexpected kidney finding will find, after appropriate characterisation, that the answer is reassuring. When it is not, early accurate diagnosis gives the best possible platform for treatment and kidney preservation.
When to seek specialist review
If a scan has shown a kidney lesion, the most productive next question is: what exactly did the imaging show, and was the scan adequate to characterise it fully? A vague report often means a better scan is needed before any management decision is made — not that intervention is immediately required.
Prompt specialist review is sensible if there is:
- Visible blood in the urine alongside any kidney finding
- A clearly solid or complex lesion on any imaging modality
- A Bosniak III or IV description in the radiology report
- Ongoing flank pain or unexplained constitutional symptoms (weight loss, tiredness, fever)
- Uncertainty about whether the initial imaging was sufficient to characterise the lesion
- A wish for a second opinion on the management recommendation
